Maximizing Patient Retention: Proven Strategies for Healthcare Practices

Patient retention is the quiet engine behind sustainable healthcare practice growth. When patients consistently show up, follow care plans, and return for preventive visits, your schedule stabilizes, your team’s workload becomes more predictable, and outcomes improve, which is crucial for ${anchorText}. The best part: improving retention often costs less than acquiring new patients—because you’re optimizing experiences for people who already trust you.
In this guide, you’ll find proven, practical patient retention strategies you can implement across the patient journey—phone calls, intake, follow-ups, and ongoing communication—plus ways to measure what’s working and where patients are slipping away.
Why patient retention matters more than ever
Retention isn’t just a business metric; it’s a clinical and operational advantage.
- Better outcomes: Patients who stay engaged are more likely to complete treatment plans, adhere to medications, and attend follow-ups.
- More predictable revenue: Retained patients reduce last-minute schedule gaps and improve capacity planning.
- Lower marketing pressure: Strong patient loyalty reduces the need to constantly “refill the funnel.”
Industry benchmarks vary by specialty, but many practices aim to keep annual patient churn in the single digits to low teens. Even small improvements compound over time because each retained patient can lead to future visits, referrals, and higher lifetime value.
The hidden cost of churn
Churn shows up in places that don’t always get tracked:
- Unreturned voicemail messages
- Patients who never complete registration
- No-shows that aren’t rebooked
- Missed follow-ups after labs, imaging, or referrals
- Poor handoffs between front desk and clinical staff
If you want to quantify the upside of reducing churn, start with two quick baselines:
- Use the Patient Lifetime Value Calculator to estimate what a retained patient is worth over time.
- Use the Practice Growth Calculator to model how incremental improvements in retention affect revenue and capacity.
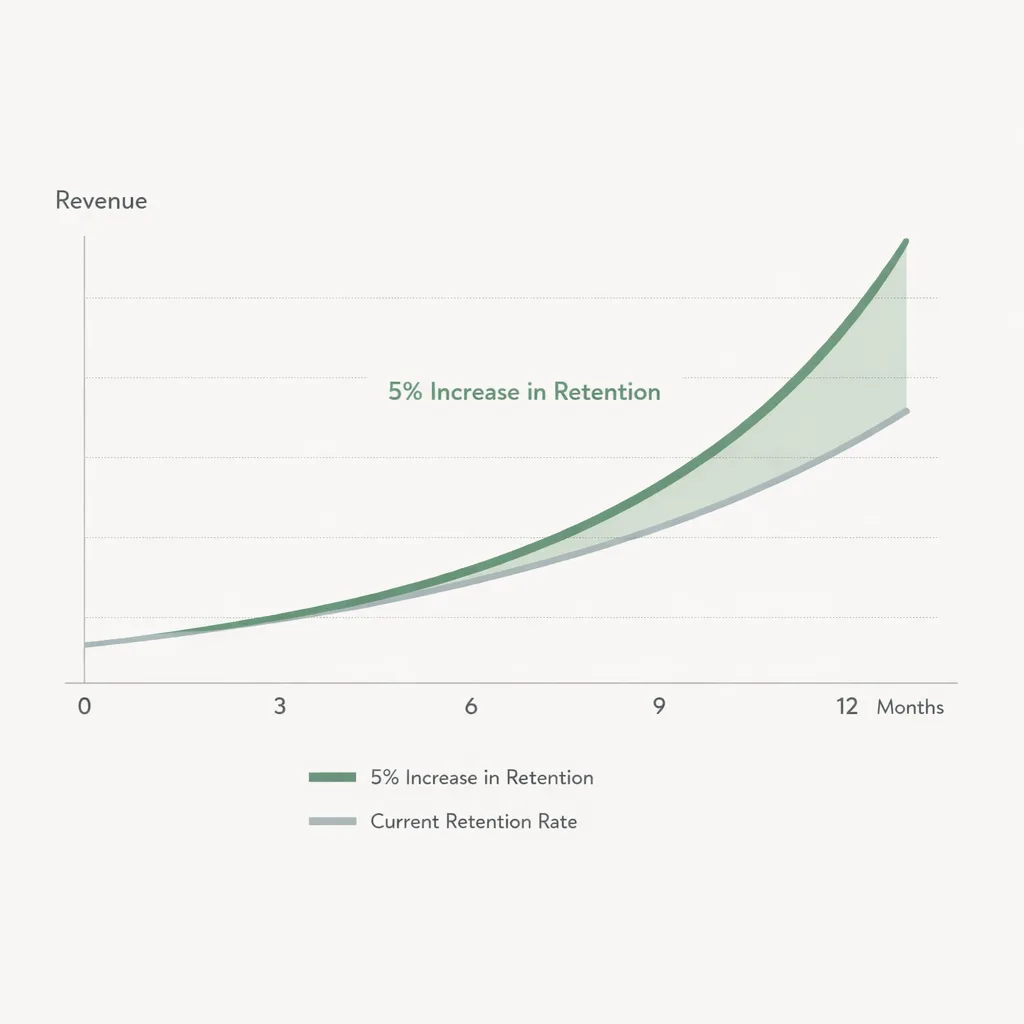
Map the retention journey: where patients decide to stay (or leave)
Retention is the result of dozens of small experiences. A helpful way to improve it is to map the journey into “decision moments” and assign an owner and metric to each.
The 6 decision moments that drive patient loyalty
- First contact: How quickly calls/messages are answered, and whether the patient feels understood.
- Scheduling: How easy it is to find an appointment time that fits their life.
- Intake: How much friction exists in forms, insurance, and instructions.
- Visit experience: Wait time, clarity, empathy, and next steps.
- Follow-up: Whether the patient receives reminders, results, and rebooking prompts.
- Ongoing communication: Proactive outreach, education, and responsiveness between visits.
If your practice is struggling with any of the first three moments, start there—because patients can’t be retained if they never successfully become established.
For intake-specific improvements, see FrontDesk’s New Patient Intake workflow.
Strategy 1: Make access effortless (speed + convenience wins)
Access is the foundation of patient retention strategies. Patients stay loyal to practices that respect their time.
Reduce call friction and missed connections
Many practices still lose patients because:
- Calls go to voicemail during peak hours
- Hold times exceed a patient’s patience threshold
- Staff can’t keep up with repetitive scheduling questions
An AI-powered receptionist can help capture more opportunities without burning out your team—especially after-hours, during lunch, and during call surges.
FrontDesk can support common access tasks like:
- Answering routine questions (hours, location, services)
- Scheduling and rescheduling
- Routing urgent calls appropriately
- Capturing complete patient details for follow-up
If you want scripts and best practices for converting first-time callers into booked appointments (and keeping them), use New Patient Calls That Convert.
Offer fast rescheduling to prevent drop-off
Patients often churn after one poor scheduling experience. Build a “rescue path” for cancellations:
- Send a reschedule link or callback option immediately
- Offer a short list of nearby openings
- Prioritize rebooking within 7–14 days (where clinically appropriate)
Strategy 2: Fix intake friction (the #1 preventable leak)
Intake is where motivated patients can become frustrated patients. Every extra step—duplicate forms, unclear instructions, long waits to confirm insurance—creates drop-off risk.
Streamline intake with a checklist mindset
Use a standardized intake checklist for every new patient:
- Required demographics and contact preferences
- Insurance details and eligibility checks
- Consent forms (HIPAA, financial policy)
- Visit expectations (arrival time, what to bring)
- Clear next steps if they have questions
When intake is consistent, patients feel confident and cared for.
For a real-world example in behavioral health, review Clarity Mental Health Intake to see how reducing intake friction improved the patient experience.

Strategy 3: Use proactive outreach (don’t wait for patients to remember)
Patients rarely churn because they “don’t like you.” More often, life gets busy and care falls off their radar.
Proactive outreach turns retention into a system.
Build outreach campaigns around high-impact moments
Common retention campaigns include:
- No-show recovery: Same-day message + easy rebooking options
- Post-visit follow-up: “How did it go?” plus next-step scheduling
- Care gaps: Annual physicals, chronic care check-ins, preventive screenings
- Lapsed patient reactivation: Patients not seen in 12–18 months
FrontDesk’s Patient Outreach tools can help automate reminders and follow-ups while keeping messaging consistent and compliant.
Use a simple cadence (and stick to it)
A practical starting cadence:
- Day 0: Appointment confirmation + prep instructions
- Day -2 to -1: Reminder + easy reschedule option
- Day +1: Thank-you + satisfaction check
- Day +7 to +14: Follow-up prompt if next visit is recommended
Strategy 4: Personalize communication without adding staff workload
Personalization is a major driver of patient loyalty—but it doesn’t require handwritten notes. It requires using the right data and being consistent.
Centralize patient context with a CRM
When staff have to hunt for context, patients feel it. A dedicated system helps your team see:
- Preferred name and communication channel
- Prior visit history and open tasks
- Appointment patterns and no-show risk
- Outstanding follow-ups
FrontDesk’s Patient CRM is designed to keep patient conversations, tasks, and outcomes organized—so every interaction feels informed.
Segment patients for more relevant outreach
Start with 3–5 segments you can act on:
- New patients (first 30 days)
- Chronic care patients (quarterly touchpoints)
- High no-show risk (extra reminders)
- Lapsed patients (reactivation)
- Post-procedure / post-therapy (outcome and plan adherence)
Strategy 5: Measure experience continuously (and close the loop)
You can’t improve what you don’t measure—and patient experience is often measured too late (or not at all).
Use a lightweight satisfaction survey
A short survey after key visits can reveal patterns early:
- “How easy was it to schedule?”
- “Did you feel listened to?”
- “Were next steps clear?”
- “How likely are you to recommend us?”
Start with the Patient Satisfaction Survey and customize it to your specialty.
Close the loop within 48 hours
Retention improves when patients see that feedback leads to action.
- Assign an owner to review responses daily
- Call back dissatisfied patients quickly
- Document the fix (and the outcome)
Strategy 6: Reduce no-shows with systems, not guilt
No-shows are a retention problem in disguise. If you only enforce fees without improving the system, patients may leave.
Focus on the “why” behind missed visits
Common causes include:
- Confusing appointment instructions
- Transportation or childcare issues
- Anxiety (especially in mental health)
- Long wait times between scheduling and visit
- Financial uncertainty
Solve the operational causes first, then apply policies fairly and consistently.
No-show reduction playbook
- Send reminders with one-tap confirmation
- Include clear location/parking info
- Offer telehealth when clinically appropriate
- Provide easy rescheduling paths
- Track no-shows by provider, time, and visit type
For an example of retention gains in a therapy setting, see ActiveLife PT Retention.
Strategy 7: Align front desk workflows with clinical care
Patients experience your practice as one system. If the front desk is overwhelmed, clinical care feels disorganized—even when it’s excellent.
Build a “handoff standard” for next steps
Before a patient leaves (or ends a call), confirm:
- What happens next
- Who to contact with questions
- When they should schedule again
- What to do if symptoms worsen
This is especially important in high-throughput environments like Urgent Care Solutions, where patients may not have an established relationship yet.
Prepare for call spikes
Call volume spikes can tank retention when patients can’t reach you.
A real example: FamilyFirst Primary Care Call Volume shows how practices can reduce missed calls and improve responsiveness during peak demand.
Strategy 8: Use analytics to find retention leaks (and prioritize fixes)
Retention work becomes much easier when you can see where patients drop.
FrontDesk’s Practice Analytics can help practices monitor operational signals like:
- Answer rates and missed call patterns
- Booking conversion rates
- No-show and cancellation trends
- Follow-up completion rates
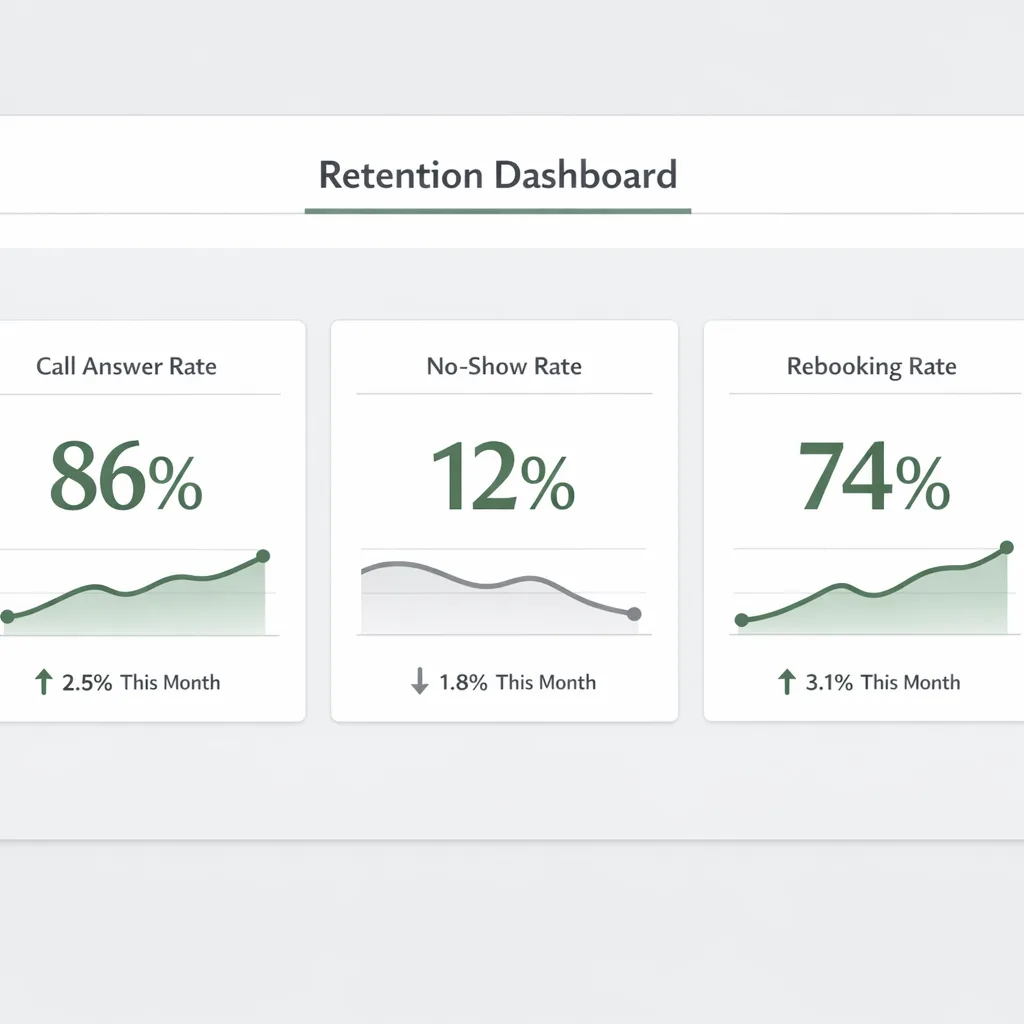
A simple retention dashboard (what to track weekly)
Track a small set of metrics consistently:
| Metric | Why it matters | Good starting target | First fix if low |
|---|---|---|---|
| Call answer rate | Missed calls = lost patients | 85–95%+ | Add coverage during peaks, AI receptionist support |
| Booking conversion rate | Measures how well inquiries become visits | 60–80%+ | Improve scripts, reduce hold time, simplify scheduling |
| Intake completion rate | Intake friction predicts churn | 85–95%+ | Shorten forms, clarify instructions, send reminders |
| No-show rate | No-shows reduce outcomes + loyalty | Varies by specialty (often <10%) | Improve reminders, confirm barriers, offer rescheduling |
| Rebooking rate | Indicates continuity of care | Increase month over month | Standardize next-step scheduling at checkout |
Targets vary by specialty and patient population, but the key is consistency: measure weekly, act monthly.
Strategy 9: Tailor retention approaches by specialty
Different specialties have different retention drivers. Here are a few practical adaptations.
Primary care: emphasize continuity and preventive care
In Primary Care Solutions, retention improves when patients feel your practice “remembers” them.
- Automate annual wellness visit outreach
- Close care gaps (labs, screenings, chronic care)
- Offer same-day or next-day options for acute needs
Mental health: prioritize trust, privacy, and low-friction communication
In Mental Health Solutions, retention is closely tied to emotional safety and consistency.
- Make rescheduling easy (reduces shame and drop-off)
- Use supportive reminders and clear expectations
- Reduce administrative burden so clinicians can focus on care
Urgent care: convert episodic visits into ongoing relationships
Urgent care retention often means:
- Capturing accurate contact info every time
- Offering follow-up options (PCP referral, recheck visits)
- Sending post-visit instructions and a satisfaction check
Strategy 10: Choose technology that supports humans (not more tabs)
Technology should reduce workload and improve responsiveness—not add steps.
When evaluating tools, look for:
- Clear ROI (time saved, calls captured, no-shows reduced)
- Easy staff adoption
- Reporting that ties to retention metrics
- Patient-friendly communication
If you’re comparing platforms, FrontDesk’s FrontDesk vs Luma Health page breaks down key differences that matter for practice operations and patient engagement.
Implementation plan: improve retention in 30 days
If you want momentum without overwhelming your team, use this phased approach.
Week 1: Diagnose and pick one “leak”
- Review missed calls, no-shows, and intake drop-offs
- Identify your biggest bottleneck (one only)
- Set a baseline metric
Week 2: Standardize scripts + workflows
- Create a scheduling script and a reschedule script
- Define next-step handoff standards
- Train staff for consistency
Week 3: Launch outreach and feedback loops
- Start no-show recovery outreach
- Send post-visit satisfaction surveys
- Assign an owner to close the loop
Week 4: Measure results and expand
- Compare metrics to baseline
- Keep what worked, remove what didn’t
- Expand to the next biggest leak
Frequently Asked Questions
What are the most effective patient retention strategies for small practices?
Focus on access and follow-up: answer more calls, reduce intake friction, and proactively rebook patients before they disappear. Small practices often see quick wins by standardizing scripts and automating reminders. Measure one or two metrics weekly so improvements don’t fade.
How do I calculate patient lifetime value for my clinic?
Patient lifetime value typically includes average visits per year, average revenue per visit, and the average number of years a patient stays with your practice. You can estimate it quickly using the Patient Lifetime Value Calculator. Use it to prioritize retention work where it has the biggest financial impact.
What’s a good patient retention rate in healthcare?
It depends on specialty, patient population, and whether visits are episodic or longitudinal. Rather than chasing a universal benchmark, track your own retention and churn trends over time and aim for steady improvement. Pair retention rate with rebooking and no-show metrics for a clearer picture.
How can we improve patient loyalty without hiring more front desk staff?
Automate repetitive tasks (scheduling, reminders, basic FAQs) and centralize patient context so every interaction is faster and more personal. Tools like AI reception and a patient CRM reduce time spent on back-and-forth while improving responsiveness. The goal is to let staff focus on complex, human conversations.
How often should we send patient satisfaction surveys?
Send short surveys after high-impact moments: first visits, annual visits, post-procedure follow-ups, and after a resolved complaint. Keep it brief so response rates stay high, and respond to negative feedback within 48 hours. Start with the Patient Satisfaction Survey and adjust questions based on what you’re trying to improve.
Conclusion: retention is a system you can build
Patient retention doesn’t come from one tactic—it comes from reliable access, low-friction intake, consistent follow-up, and communication that makes patients feel known. When you operationalize those elements with measurable workflows, patient loyalty rises naturally—and so does healthcare practice growth.
If you’re ready to capture more calls, reduce intake drop-off, and run smarter outreach without adding chaos to your day, FrontDesk can help you put these patient retention strategies into motion. Explore FrontDesk’s tools like Patient Outreach, Patient CRM, and Practice Analytics to start building a retention engine your team can sustain.