Understanding the Patient Journey: Streamlining Experiences from First Contact to Follow-Up

Every phone call, web form, text message, and check-in shapes how patients feel about your practice—often before they ever meet a clinician. The “patient journey” isn’t just a marketing concept; it’s the operational reality that determines schedule fill rate, staff workload, reviews, and long-term retention. When you streamline patient engagement from first contact to healthcare follow-up, you reduce friction, improve patient experience, and protect revenue.
This article breaks the journey into practical stages, shows where most practices lose patients, and provides an actionable playbook—especially for healthcare practice owners and office managers who need systems that work on busy days.
What the patient journey really means (and why it matters)
The patient journey is the full set of interactions a patient has with your practice—from the moment they discover you to the messages they receive after care. It includes both clinical and non-clinical touchpoints, but most “experience leaks” happen in operational moments: unanswered calls, confusing intake, unclear pricing, and inconsistent follow-up.
A strong journey matters because:
- Patients increasingly behave like consumers: they compare options, read reviews, and expect fast responses.
- Access and communication are leading drivers of satisfaction; long hold times and delayed callbacks are common reasons patients switch.
- Retention is economically powerful: a returning patient often has higher acceptance and lower acquisition cost than a brand-new one.
To quantify the upside of improving retention and follow-up, use FrontDesk’s Patient Lifetime Value Calculator to estimate how much each retained patient is worth over time.
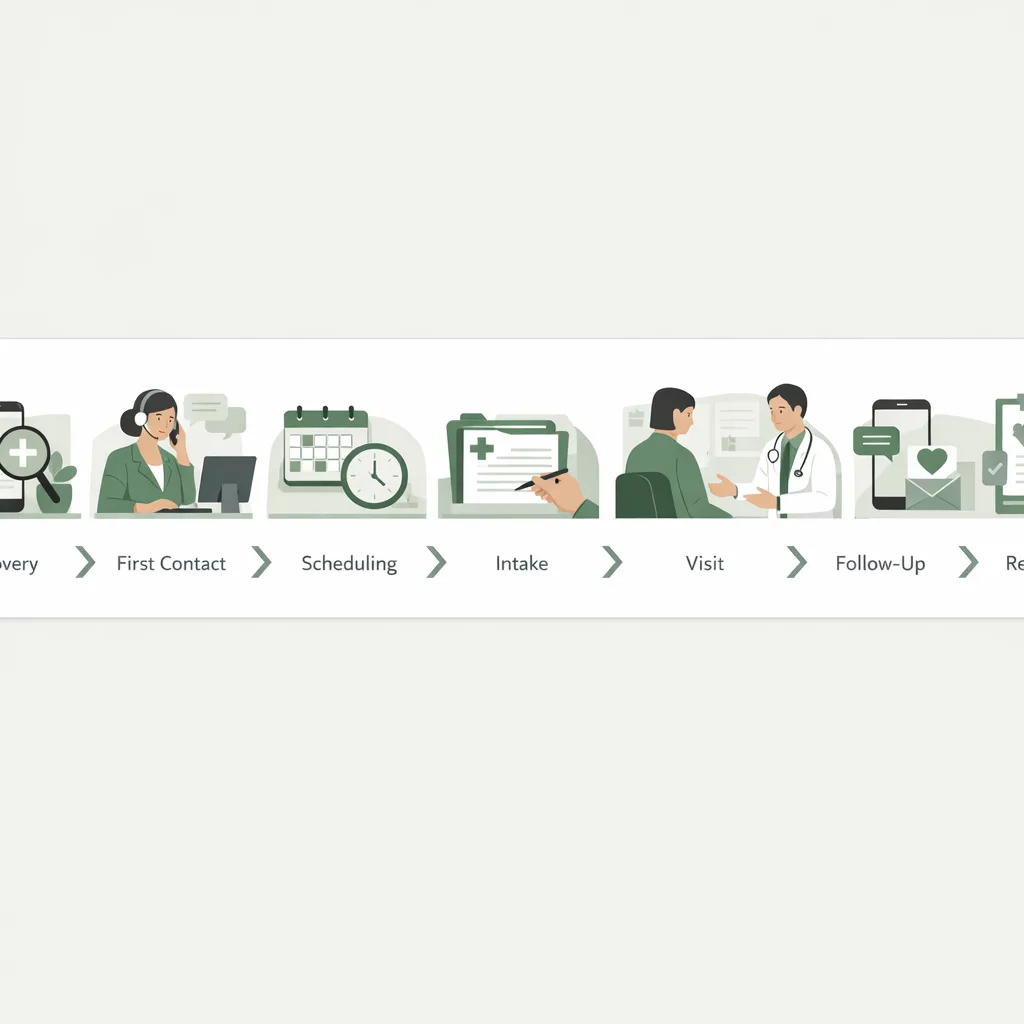
The 7 stages of the patient journey (with common friction points)
Think of the journey as seven connected stages. If any stage breaks, patients feel it—and staff ends up patching gaps manually.
1) Discovery and first impression
What patients do: search online, read reviews, ask friends, visit your website.
Common friction: inconsistent hours, unclear services, no “what to expect,” hard-to-find phone number.
Actionable improvements:
- Put clear next steps on your site: “Call or text to schedule,” “New patient forms,” “Insurance info.”
- Ensure voicemail and auto-replies set expectations (“We’ll respond within X minutes/hours”).
- Standardize your service descriptions and eligibility requirements (who you treat, referral needs, etc.).
2) First contact (call, text, web form)
What patients do: test how responsive you are.
Common friction: missed calls, long hold times, phone tag, inconsistent scripting.
Actionable improvements:
- Use a consistent call structure for new patient inquiries. FrontDesk has a practical guide, New Patient Calls That Convert, plus a ready-to-use New Patient Call Script to reduce variability.
- Offer multiple contact methods (phone + SMS) and respond quickly—speed is a competitive advantage.
- Track “source” (Google, referral, insurance directory) so you can invest in what works.
If your team struggles to keep up with inbound volume, FrontDesk’s AI receptionist can help capture intent, answer common questions, and route requests—so fewer leads fall through the cracks.
3) Scheduling and pre-visit communication
What patients do: decide whether booking feels easy and trustworthy.
Common friction: limited availability, unclear cancellation policy, confusing instructions, anxiety about the visit.
Actionable improvements:
- Send confirmations and reminders via SMS and email.
- Include a “what to bring” checklist and parking/arrival instructions.
- Reduce pre-appointment anxiety with clear expectations. See The Role of AI in Reducing Patient Anxiety Before Appointments for practical messaging ideas.
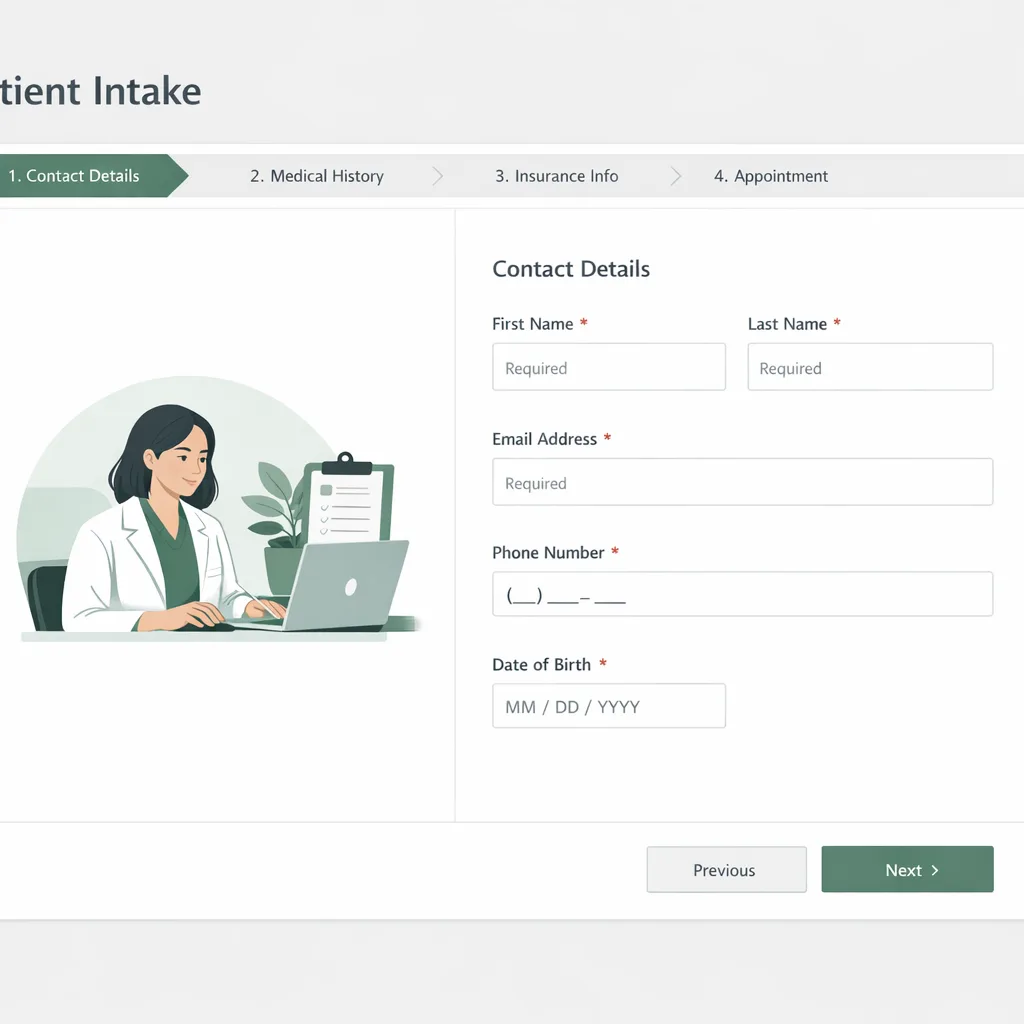
4) New patient intake (forms, insurance, consent)
What patients do: provide information—often repeatedly.
Common friction: paper forms, duplicate data entry, missing fields, last-minute surprises.
Actionable improvements:
- Digitize intake and send it early.
- Use standardized templates so nothing is missed.
FrontDesk’s New Patient Intake workflow is designed to reduce back-and-forth and help patients complete intake before they arrive. You can also start with proven templates like Patient Intake Forms and learn best practices in The Ultimate Guide to Digital Forms: Streamlining Patient Intake and Documentation.
5) Check-in, wait, and the in-office experience
What patients do: evaluate professionalism and respect for their time.
Common friction: long waits without updates, unclear payment expectations, staff interruptions.
Actionable improvements:
- Set expectations: “You may wait up to X minutes; we’ll update you if we’re running behind.”
- Provide a simple payment explanation (copay, deductible, self-pay estimates).
- Train staff on “micro-moments”: greeting by name, confirming pronunciation, offering next steps.
6) Post-visit next steps (care plan + scheduling continuity)
What patients do: decide whether to follow through.
Common friction: vague instructions, no next appointment booked, difficulty reaching the office after the visit.
Actionable improvements:
- Before the patient leaves, confirm:
- What happens next
- When they should return
- How to contact you with questions
- Send a short recap message (non-clinical summary + logistics).
- For multi-visit care (PT, chiropractic, behavioral health), pre-schedule a series when possible.
For retention strategies that support ongoing care plans, see Maximizing Patient Retention: Proven Strategies for Healthcare Practices and the focused guide Physical Therapy Patient Retention.
7) Healthcare follow-up and long-term relationship
What patients do: judge whether you remembered them and whether care actually continues.
Common friction: no follow-up after missed appointments, inconsistent reactivation, no feedback loop.
Actionable improvements:
- Build a follow-up cadence for:
- No-shows/cancellations
- Post-procedure check-ins
- Inactive patients (e.g., 60–180 days)
- Review requests (when appropriate)
- Use structured messaging and track outcomes.
FrontDesk supports proactive re-engagement with Patient Outreach, while Patient CRM helps you organize patient communication history and segment follow-ups so outreach is timely—not spammy.
A streamlined patient journey blueprint (copy/paste for your practice)
Use this blueprint to map your current process and identify the biggest gaps.
Step 1: Map touchpoints and owners
List each touchpoint, the channel, who owns it, and what “good” looks like.
Step 2: Define service-level targets (SLAs)
Operational targets reduce ambiguity and help you staff appropriately. Examples:
- Answer or return missed calls within 15 minutes during business hours
- Send appointment confirmation immediately after scheduling
- Send intake link within 5 minutes of booking
- Follow up on no-shows within 30 minutes
Step 3: Standardize scripts and templates
Standardization improves patient experience and reduces staff stress. Start with:
- New patient inquiry script (New Patient Call Script)
- Intake packet templates (Patient Intake Forms)
- Feedback request templates (see below)
Step 4: Automate “repeatable” communication
Automate reminders, intake nudges, and follow-ups—then reserve human time for exceptions and empathy.
A helpful reference on communication best practices is Leveraging AI for Effective Patient Communication: Best Practices for Growth.
Step 5: Measure, then iterate monthly
Pick a small set of metrics, review them monthly, and adjust.
Metrics that reveal where the patient experience is breaking
You don’t need dozens of dashboards—just the metrics that connect operations to outcomes.
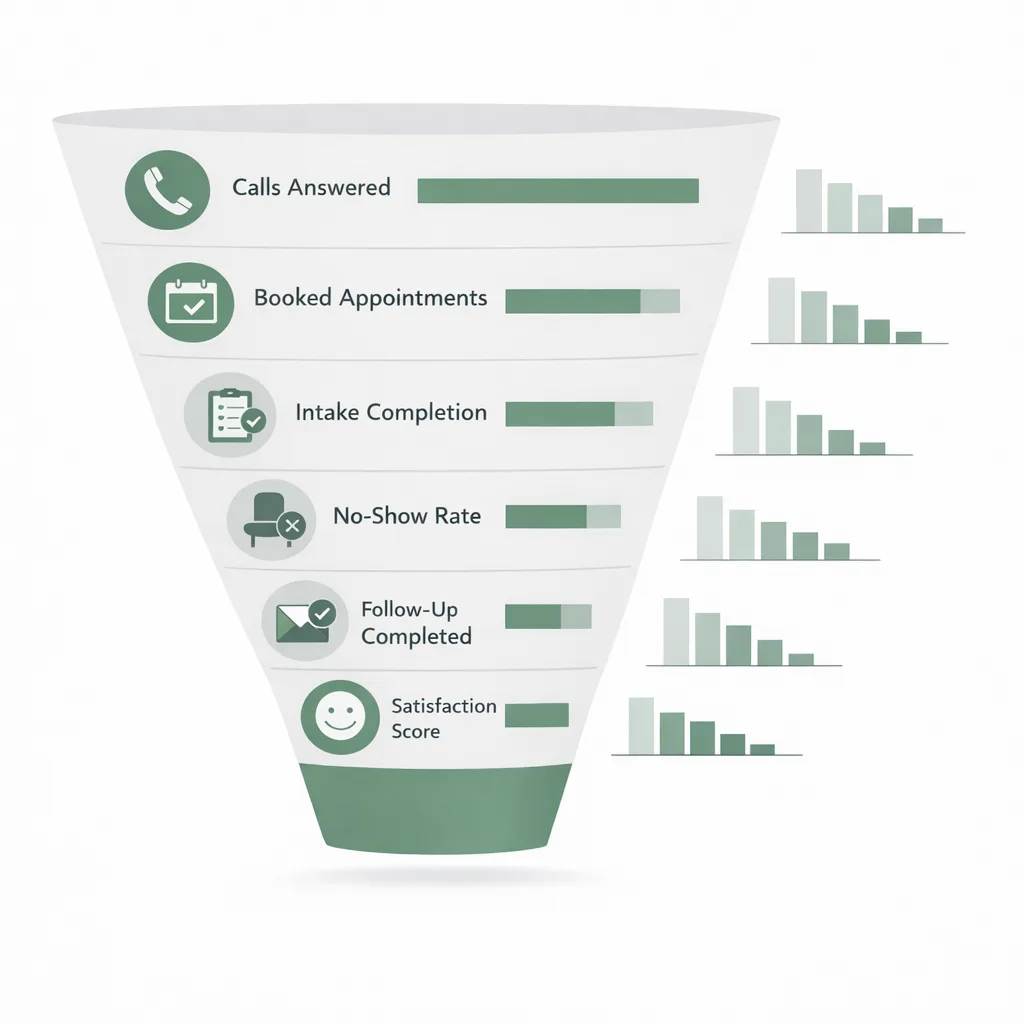
| Patient journey stage | Metric to track | What “good” looks like | Common fix when it’s low |
|---|---|---|---|
| First contact | Call answer rate / speed to respond | High responsiveness during open hours | Add overflow handling, tighten scripts, improve routing |
| Scheduling | Lead-to-appointment conversion | Steady week over week | Reduce friction, offer clearer availability, follow up on missed calls |
| Intake | Intake completion rate before visit | Majority completed pre-visit | Send forms earlier, add reminders, simplify required fields |
| Visit | No-show rate | Trending down | Improve reminders, confirm barriers, offer easy rescheduling |
| Follow-up | Follow-up completion rate | Consistent outreach for cancellations/no-shows | Create automated sequences and clear ownership |
| Experience | Satisfaction score / reviews | Stable and improving | Close the loop on issues, train front desk on empathy |
To collect structured feedback, use FrontDesk’s Patient Satisfaction Survey or start with a template like Patient Satisfaction Survey. Even a short 3–5 question survey can highlight bottlenecks you can fix quickly.
Where AI fits: reducing friction without losing the human touch
AI should remove busywork, not replace empathy. In practice management, the best use cases are repetitive, time-sensitive interactions that otherwise create phone tag and delays.
High-impact AI use cases in the patient journey
- Capturing missed calls and after-hours inquiries so patients don’t drift to competitors
- Answering common questions (hours, location, services, insurance basics)
- Routing messages to the right team member with context
- Automating reminders and follow-ups with consistent tone and timing
- Logging interactions so staff sees the full story without digging
FrontDesk is built for these workflows—helping practices respond faster and keep communication organized, which directly improves the patient experience.
Practical playbooks for common breakdowns
Below are quick, operational fixes you can implement this week.
Playbook: Missed calls → lost patients
- Audit when calls are missed (lunch, peak hours, after-hours).
- Implement a same-day callback standard (e.g., within 15–30 minutes).
- Use a conversion-focused intake script and track outcomes.
- Review weekly: missed calls, callback time, booked rate.
If you want help designing a call flow that converts, start with New Patient Calls That Convert.
Playbook: Intake delays → late starts and staff overload
- Send digital forms immediately after booking.
- Add automated reminders at 48 and 24 hours pre-visit.
- Make required fields truly required (avoid “we’ll fix it at check-in”).
- Provide a “help” option for patients who get stuck.
Playbook: No-shows → schedule instability
- Confirm appointment details and reduce uncertainty (location, parking, cost expectations).
- Use two-way messaging so patients can reschedule instead of disappearing.
- Follow up quickly after a missed appointment with a clear next step.
Playbook: Weak healthcare follow-up → low retention
- Segment follow-up by scenario (post-visit, no-show, inactive, satisfaction issue).
- Assign ownership (who sends what, when).
- Maintain continuity by referencing prior conversations (this is where a CRM view helps).
Frequently Asked Questions
What is the patient journey in a healthcare practice?
The patient journey is the end-to-end experience a patient has with your practice, from discovery and first contact through the visit and healthcare follow-up. It includes operational touchpoints like scheduling, intake, reminders, and post-visit communication. Improving these moments reduces friction and increases retention.
How can I improve patient experience without adding staff?
Start by standardizing scripts and templates, then automate repeatable communication like reminders, intake nudges, and follow-ups. Tools like a dedicated CRM and outreach workflows help teams respond faster and stay consistent. The goal is to reserve staff time for complex questions and empathy-driven conversations.
What should a good healthcare follow-up process include?
A strong follow-up process includes timely outreach for no-shows and cancellations, post-visit check-ins when appropriate, and reactivation messages for inactive patients. It should be consistent, trackable, and tailored by patient segment. Avoid one-size-fits-all blasts—patients respond better to relevant, contextual messages.
Which metrics best indicate problems in the patient journey?
Look at call answer rate, speed to respond, lead-to-appointment conversion, intake completion before the visit, no-show rate, and patient satisfaction trends. These metrics map directly to where patients feel friction. Review them monthly and choose one bottleneck to fix at a time.
How do I collect patient feedback effectively?
Keep surveys short (3–5 questions), send them soon after the visit, and include at least one open-ended question. Use a structured tool like the Patient Satisfaction Survey to track trends over time. Most importantly, close the loop with patients when feedback reveals an issue.
Conclusion: Make the journey your competitive advantage
When you treat the patient journey as an operational system—not a vague concept—you make it easier for patients to choose you, show up, and stay with you. Small improvements at first contact, intake, and healthcare follow-up often create outsized gains in schedule stability, reviews, and retention.
If you want to streamline communication, reduce missed opportunities, and build a more consistent patient experience, FrontDesk can help. Explore how our AI receptionist and workflows fit your practice—or reach out via Contact to see it in action.